Opioid Addiction is a disease, not a moral failing.
You were strong enough to survive your addiction, and you’re more than strong enough to recover from it.
Send us a message or call (844) 535-7291 to get help now.
Whatever brought you to us, we’re glad you’re here
You’re starting your personal journey to recover. You might feel alone, but you’re about to find a whole team — an entire community — that is ready to welcome you. You might feel beaten up, but you aren’t beaten down. You got yourself here, and you still have fight left in you.
There’s a lot of work to do together, but we know you can do it. There is nothing wrong with you that can’t be fixed by what’s right with you.
We deliver real recovery℠.

Substance use disorder (commonly known as drug addiction) is recognized by the American Medical Association and other authorities as a medical disease that upsets normal brain function. Some have compared substance use disorder with other illnesses, such as diabetes — it doesn’t go away on its own, and only gets worse without proper treatment.
At Behavioral Health Group (BHG), we understand that the path of recovery from opioid abuse will look different for each individual. We don’t believe in treatment for treatment’s sake. Recovery is the goal, treatment is how you get there, and medication makes treatment possible.
If you feel that you are wanting to take that step to better yourself, and have the things that you want in life, and do the things that you want, make a phone call to BHG. It will definitely change your life. It changed mine.
Nichole P.
Click to WatchReady to get help now?
Our comprehensive approach

BHG incorporates a breadth of services to meet patients where they are and stay with them on their recovery journey, connecting them to the appropriate resources and services to ensure they have every opportunity for success and well-being.
During the course of treatment and recovery, each patient requires a unique combination of services and treatment components. For example, in addition to counseling or psychotherapy, a patient may require medication, medical services, family therapy, parenting instruction, vocational rehabilitation, and/or social and legal services.
Our expansive counseling services and focus on case management deliver better guidance and consultation to patients and family members. Additionally, by offering OTP (opioid treatment programs) and OBOT (office-based opioid treatment) in multiple locations, we’re able to be flexible with medication types and how they’re administered.
Medication-assisted treatment
As part of a comprehensive treatment program, BHG can administer — or in some cases, prescribe — medications that are FDA approved for the treatment of opioid use disorder.
According to the National Institute on Drug Abuse (NIDA), “taking these medications as prescribed allows patients to hold jobs, avoid street crime and violence, and reduce their exposure to HIV by stopping or decreasing injection drug use and drug-related high-risk sexual behavior. Patients stabilized on these medications can also engage more readily in counseling and other behavioral interventions essential to recovery.”
It’s important to note that BHG provides comprehensive opioid use disorder recovery services, and offers medication — we are not “medication only.”
Some patients come to us knowing that they want medication, while others just know that they want to get better. If you’re not sure how you feel about medication, we’re ready to support your treatment and recovery in whatever way works for you.
Yes. Numerous research studies conducted over nearly 60 years have repeatedly shown that medications are effective in the treatment of opioid use disorder. Further, medications have been shown to help people stay in treatment so they have the opportunity to get into recovery.
Unfortunately, many people do not receive the treatment they need, either due to lack of access to providers, or due to misconceptions and stigmas about MAT programs.
This is a common misconception, but it doesn’t reflect the reality of what MAT actually does and how the medications work. When a patient receives MAT, they are moving from using opioids in an unsafe, destructive, and often illicit manner, to using a highly regulated medication that has been FDA approved for the specific purpose of treating addiction.
At BHG treatment centers, medication is administered under the care of trained physicians and medical professionals. Additionally, the medications used in our Medication-Assisted Treatment programs are pharmacologically different from commonly abused pain pills or heroin. These FDA-approved medications provide relief from the physical withdrawal symptoms and cravings associated with opioid dependence, while preventing the euphoric effects of other opioids.
Addiction counseling and therapy

Support services such as counseling and behavioral interventions are fundamental components to all BHG programs. With the support provided by our counseling team and clinicians, patients learn how to better recognize triggers, develop coping skills, and improve their overall mental health.
Our counselors meet patients wherever they are in their journey and collaborate with them to create short-term and long-term goals as part of an individualized treatment plan.
Behavioral therapy
Behavioral therapies vary in their focus and may involve addressing a patient’s motivation to change, providing incentives for abstinence, building skills to resist drug use, replacing drug-using activities with constructive and rewarding activities, improving problem-solving skills, and facilitating better interpersonal relationships.
Group therapy
Group treatment is often preferred for people with opioid use disorder. It makes use of the need to belong and the healing power of human connections. The group helps patients feel less isolated and ashamed, and allows them to help themselves by helping others. Groups can provide both emotional support and confrontation, along with information and understanding.
Individual therapy sessions
In individual therapy sessions, clients often dig deeper into the work done in group therapy, allowing them to spend more time on individual issues. Patients work with their dedicated counselor to build a close, honest relationship based on mutual trust and commitment to recovery.
Family counseling
Where possible, it is important to enlist the patient's family. Relatives can be coached on how to confront the patient or taught how to facilitate cognitive and behavioral therapy. In a variant called network therapy, friends and relatives become part of the therapeutic team, meeting to discuss what to do in relapses and other emergencies.
Your questions, answered
The first step is yours. Simply walk in to any of our treatment centers. You'll have an assessment done by one of ourcounselors. The first assessment makes sure our program is right for you, and that we can meet your specific needs. There are also a physical health assessment and a physical exam and some laboratory tests we'll need.
If the program is right for you, you'll get some medication and the process of treatment will be underway. Soon, you'll have another assessment, designed to get to know you as an individual.
The information you provide us over all these assessments will be used to create an individualized treatment plan (ITP).
Read LessLike many chronic conditions, such as diabetes, high blood pressure, or asthma, SUD is something that can be effectively treated and managed, rather than ‘cured.’ Thousands of people find long-term stability and recovery through participation in medication assisted recovery combined with behavioral counseling.
All BHG services are provided in an outpatient setting. This allows the you to receive treatment while you continue to live at home, attend work or school, and live a normal life. We also provide counseling through telehealth so that you have the most flexibility connecting and getting support on your recovery journey.
Addiction takes many things from people: their family, friends, jobs, their physical and mental health, their freedom. For some people, addiction takes everything.
Stopping substance use (getting sober) is just a piece of recovery, because simply… Read MoreAddiction takes many things from people: their family, friends, jobs, their physical and mental health, their freedom. For some people, addiction takes everything.
Stopping substance use (getting sober) is just a piece of recovery, because simply not using substances won’t get back what you lost. Recovery is getting back what was taken, and then getting more. It isn’t about not doing something (like using substances), it’s about actively doing the things that help you live a full and fulfilling life. To get into recovery, people first need treatment.
Read LessWhen we say “treatment,” we are talking about the process that gives you the knowledge and skills you need to get into recovery. This includes group and individual counseling, as well as getting connected with healthcare services (and any other services you might need to heal).
Among other things, treatment teaches you:
- About the brain disease of addiction and the substances that cause it
- How your brain and your mind change over the course of addiction, and how to let it heal and change back
- How to identify triggers that could lead to relapse and how to avoid them
- Coping skills for getting through unavoidable, risky situations without relapsing
There are three FDA-approved medications available for the treatment of opioid use disorder: methadone, buprenorphine (Suboxone), and naltrexone.
There is no scientific evidence showing that one medication is better than the others… Read MoreThere are three FDA-approved medications available for the treatment of opioid use disorder: methadone, buprenorphine (Suboxone), and naltrexone.
There is no scientific evidence showing that one medication is better than the others. The most appropriate medication and dosage will be determined by the preferences and needs of the patient in consultation with one of our physicians.
At a proper dose, these medications do not make the person feel “drugged” or “high” like other opioids. Each dose lasts for at least 24 hours and significantly reduces drug cravings. While taking their medication as prescribed, many people say that they feel “normal” for the first time in a long time.
Read LessMethadone and buprenorphine both activate mu-opioid receptors (MORs) in the brain. However, unlike other opioids, they do so in a way that provides withdrawal symptom relief and curbs cravings while blocking the high associated with other opioids. Methadone is a “full agonist” that fully activates opioid receptors. Buprenorphine, a “partial agonist,” only partially activates opioid receptors, creating a ceiling on the medication’s effect.
In contrast to these opioid agonists, naltrexone is an opioid antagonist that simply blocks opioid receptors rather than activating them. Since opioid antagonists do not activate opioid receptors, they do not provide relief for physical withdrawal symptoms or cravings, and require full detoxification before starting treatment.
Read LessAt BHG, most treatment centers offer both in-center dosing and prescription-based programs; others offer one program only. Choose what works best for your recovery with the help of your BHG physician, nurse, and counselor...
Read MoreAt BHG, most treatment centers offer both in-center dosing and prescription-based programs; others offer one program only. Choose what works best for your recovery with the help of your BHG physician, nurse, and counselor.
In either program, you'll have the care and guidance of skilled clinicians and counselors and staff who respect you for having the courage and determination to fight back for your life through real recovery℠.
Here is a comparison of the two programs:

* The decision on which program and medication to use for each patient is a medical decision made by patients in collaboration with their BHG physician, nurse, and counselor.
Outside providers such as primary care providers or emergency room providers will not be aware of patients taking methadone in an opioid treatment program without coordination of care. We do coordinate care with other providers if the patient gives consent so that all providers are aware of treatment, chronic medical problems, and other referrals.
Read LessBHG’s Comprehensive Outpatient Experience (COPE), provides patients with intensive outpatient support.
Patients can move fluidly through different levels of care — including both Standard… Read MoreBHG’s Comprehensive Outpatient Experience (COPE), provides patients with intensive outpatient support.
Patients can move fluidly through different levels of care — including both Standard and Motivational Enhancement programs — based upon their individual needs. For example, you might transition or step down to BHG’s COPE program after completion of an inpatient or residential rehab program.
In case of relapse, COPE can also be used as a tool to help you get back on track with your recovery.
Read LessThe individualized treatment plan (ITP) is your personal roadmap to recovery. It is the document you create with your counselor that lays out your short-term and long-term goals. The ITP describes what you want in recovery, then breaks the process down into steps that we’ll take together to get you there. Through our work together, your ITP will be reviewed and updated as you accomplish your goals and make new ones. Remember: recovery is about getting back what addiction took, and then getting more.
Read LessThe short answer: long enough to rebuild healthy habits, repair relationships, and develop healthy coping strategies. Obviously, the amount of time this takes is different for everyone, and BHG does not have a “one size fits all” approach to our patients.
Some people find that medication still helps them long after they get back what they lost — and some continue to take medication indefinitely. If you find that you want to continue with the medication while you’re in recovery, we’ll be there to support you.
After treatment, some people decide to try a completely medication-free approach. If that’s what you want to do, your clinical team will work with you to help you safely make that move.
Read LessThere is no specific length of time that is best for everyone, but the longer someone stays in treatment, the greater the chances for successful recovery.
As you progress through our program, you’ll need less treatment, and you’ll see us… Read MoreThere is no specific length of time that is best for everyone, but the longer someone stays in treatment, the greater the chances for successful recovery.
As you progress through our program, you’ll need less treatment, and you’ll see us back off as your life fills back up with normal and healthy things. If there is a slip or a relapse along the way, we’ll be there to help you through it by temporarily providing more treatment until the crisis passes.
For many patients, a continuing care approach provides the best results, with the treatment intensity varying according to a person’s changing needs. When the needs of the patients go beyond what we are able to address directly, we work to connect patients to appropriate supportive services within the community.
Read LessIn addition to medical and behavioral treatment, BHG encourages abstinence from illicit substances. All patients receive scheduled and unscheduled drug tests, which are monitored by the clinic medical staff. Drug screening is not intended to be a punitive tool; rather, it helps ensure safe medication dosing, measurements of progress and accountability. This accountability, along with the constant support from the BHG medical and counseling teams, helps reduce the risk of relapse.
Read LessMethadone is an FDA-approved medication that has been used for decades to treat opioid use disorder. Methadone-assisted treatment for opioid addiction is the most researched and proven form of treatment, effective for producing positive outcomes for those struggling with opioid addiction. In fact, the World Health Organization includes methadone on its List of Essential Medicines.
The medication acts as a “full agonist” on opioid receptors within the brain and central nervous system which allows it to provide relief for severe withdrawal symptoms and helps “normalize” the brain chemistry to reduce cravings.
One of the things that sets methadone apart from other opioids is its long half-life. This means that the medication wears off much more gradually than other opioids such as morphine, fentanyl, or heroin. While the medication is able to provide relief for physical withdrawal symptoms and cravings, it blocks the euphoric high associated with other fast-acting opioids.
Because of its effectiveness, methadone-assisted treatment has been recognized as the “gold standard of care.”
Read LessResources
For Patients

Everything You Need When You Need it
To offer customized treatment and recovery you need a program that lets you choose from every service and every medication approved for substance use disorder. And you need a trusted clinical care team that knows how to get you safely started and moving successfully along your recovery pathway.

Extra Support When You Need It
For ongoing support following discharge from a residential treatment facility or enhanced support for detoxification when first entering an outpatient program for substance use disorder or additional help if experiencing a relapse or life challenge, we have the skilled counselors and programs you need.

The Benefits of Insurance
The services you receive at BHG may be covered just like any other medical costs through your health plan. In most cases, your visits to BHG are the same as visiting a primary care physician. And like other medical care there are privacy laws protecting you and your covered family members.
For Families

Helping Your Loved One
Drug addiction – officially called Substance Use Disorder – is recognized by the American Medical Association and other authorities as a medical disease that upsets normal brain function. Download this helpful resource to learn more.

Addiction and Mental Health
Addiction and mental health disorders frequently happen in people at the same time. It can be difficult to know whether a mental health condition caused the addiction, if the addiction caused the mental health problem, or if they just occurred together by coincidence. Download this helpful resource to learn more.

Treatment Points to Remember
Treatment must help patients:
- re-learn adaptive coping skills
- re-fill life with meaningful moments
- stop using drugs
Download this helpful resources to learn more.
Medication-Assisted Recovery℠ (MAR)
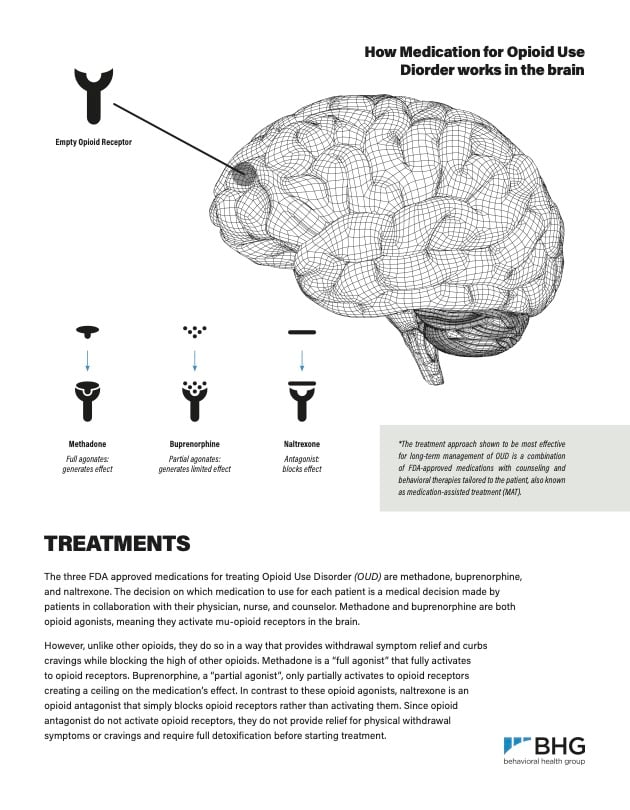
How OUD Medication Works
The three FDA approved medications for treating Opioid Use Disorder (OUD) are methadone, buprenorphine, and naltrexone. Download this helpful resource to learn how medications used in the treatment of OUD work in the brain.

OUD Medication Fact Sheet
Methadone and buprenorphine are both opioid agonists, meaning they activate mu-opioid receptors in the brain. However, unlike other opioids, they do so in a way that provides withdrawal symptom relief and curbs cravings. Download this helpful resource to learn more.
Opioid Use Disorder and Other Medical Concerns

Opioid Use Disorder and Pregnancy
While methadone and buprenorphine have both been shown to be safe and effective in pregnancy, there is a longer history, and more safety information about methadone. This is why methadone is considered “the gold standard” for OUD treatment in pregnancy. Download this helpful resource to learn more.

Opioid Use Disorder and HIV
There is no scientific evidence that ongoing medication-assisted treatment for opioid use disorder is harmful to patients with HIV or
AIDS. Nor do any of the three FDA-approved MAR medications weaken the immune system or make the illness worse. Download this helpful resource to learn more.
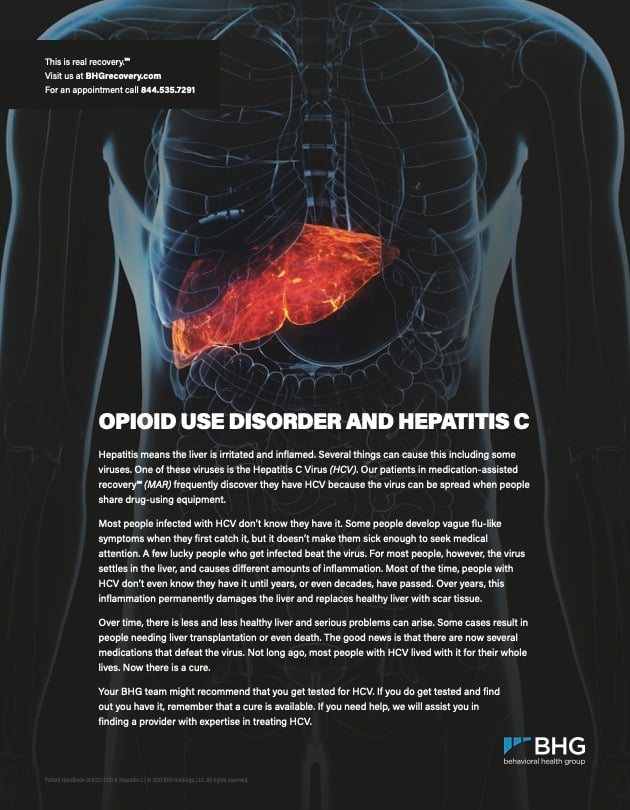
Opioid Use Disorder and HCV
Hepatitis means the liver is irritated and inflamed. Several things can cause this including some viruses. One of these viruses is the Hepatitis C Virus (HCV). Download this helpful resource to learn more.
Get better care, closer to home.
Access to personalized, outpatient treatment for opioid use disorder is now within easy reach.
Start your path to real recovery today by filling out the form or calling 844.535.7291.
[*Our calls may be recorded for quality assurance and training purposes.]

